A non-invasive,
non-narcotic,
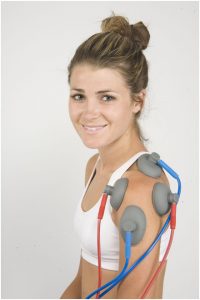
pain treatment option for your acute or chronic pain condition patients
A Brief History on this advanced electroanalgesic pain management treatment?
A wide variety of medical conditions have been successfully treated with electrical stimulation for nearly 2,000 years. Medical doctors in ancient Greece learned that the electrical impulses emitted from electric eels in clinical foot baths relieved pain and produced a favorable influence on blood circulation. Doctors Largus and Dioscorides (circa 46 SD) documented substantial therapeutic results with electrical currents in circulatory disorders and in the management of pain from neuralgia, headaches, and arthritis.
In the 1700’s, European physicians used controlled electrical currents from electrostatic generators almost exclusively for numerous medical problems involving pain and circulatory dysfunction. During that period, Benjamin Franklin also documented pain relief by using electrical currents for “frozen shoulder.”
By the late 1800’s, more than 50% of all American physicians used some form of electromedicine in their practices daily for many different medical problems, including the management of pain and wound healing.
In 1910, an incorrect, misleading, and unfair report was published by powerful, biased special-interest groups discrediting the value of electrical treatments and nutritional therapy in the human body. Within months, the fear of personal condemnation from certain medical organizations (funded by the special interest groups) forced American physicians to nearly abandon electromedical treatment and nutritional therapy from their private practices.
The modern age of clinical electromedicine actually began in Germany around 1950, when electrical signals or impulses were able to be generated that mimicked the electrical impulses which naturally occur in all of our bodies.
Using this different type of electrical current, medical electrical treatments could be applied very comfortably to human skin, while therapy could be delivered to much deeper tissue i.e. shoulder, hip, and low back.
Electromedical treatment gained wider acceptance in the 1960’s when medical researchers Melzak and Wall published the “Gate Control Theory of Pain.” These researchers found that certain cells in the spinal cord act as a gate through which pain travels to the brain. Overloading these neural transmitter cells will block the naturally occurring electro chemical pain impulses, thus relieving pain.
The Gate Control Theory “legitimized” electromedical treatment and once again popularized transcutaneous electric nerve stimulation (T.E.N.S.) in the United States. Typically, T.E.N.S. units are portable battery-operated devices worn continuously to apply electrical current and relieve pain by nerve counter-irritation and by releasing morphine like chemical substances in the body.
Historically, most electro medical treatments or electric stimulation therapies were developed in Europe, accepted by the medical establishment in Europe, and transferred with varying degrees of speed and acceptance to the United States.
Today, more American physicians are employing a new form of electro medicine, known as Electroanalgesia (EA).
In the last thirty years, electro-analgesic treatments have gained wide acceptance in medical teaching facilities and universities such as;

- King-Drew Medical Center, Los Angeles,CA
- Cleveland Clinic, Ohio
- Columbia University, New York
- The Cleveland Clinic Foundation, Cleveland, OH
- Loma Linda University Medical Center, Loma Linda, CA
- Charles R. Drew Univ. of Medicine &Science, LA, CA
- National Naval Medical Center, Bethesda, MD
- South Point Hospital, Warrensville, OH
- Southeast Alabama Medical Center, Dothan, AL
- N. Phoenix Health Institute, Phoenix, AZ
- DCH Regional Medical Center, Tuscaloosa, AL
In addition, the Bethesda Naval Hospital in Washington, D.C. is now successfully using electroanalgesic treatment as an effective treatment for pain management.
To most people, T.E.N.S. is synonymous with electrical stimulation. However, there are other forms of electro medicine that provide much better and longer lasting results for patients.
As a matter of difference, where T.E.N.S. impulses are 0-250 pulses per second, electroanalgesic medical devices operate at much higher frequencies (between 8,300-10,000 pulses per second).
These higher frequencies of pure alternating electrical current move through the skin quickly and efficiently with virtually no discomfort to the patient. In fact, according to numerous patients who have received electroanalgesic treatments, they have stated that they will request this treatment again and again for the potent analgesic and soothing overall relaxing effects.
The clinical uses are for the treatment of acute and chronic pain conditions.
• Stimulate peripheral nerves for the purpose of providing pain relief
• Management and symptomatic relief of chronic (Iong-term) INTRACTABLE PAIN
• Adjunctive treatment of post-traumatic pain
• Adjunctive treatment in the management of post-surgical pain
• Increasing local blood circulation
• Maintaining or increasing range of motion Muscle Re-education
• Relaxation of muscle spasms
• Prevention or retardation of disuse atrophy
• Immediate post-surgical stimulation of calf muscles to prevent venous thrombosis
CLINICAL BENEFITS
* Non-toxic, safe, and effective with minimal side effects, which result in high patient compliance and satisfaction.
Electroanalgesa (EA) treatments provide long term pain relief by releasing endorphins in the central nervous system. Endorphins are neuropeptide pain-relieving substances that occur naturally in the body. Their activation provides superior long-term pain relief.
Historically, most medical treatments or electric stimulation therapies were developed in Europe, accepted by the medical establishment in Europe, and transferred (with varying degrees of speed and acceptance) to the United States. Today, more and more knowledgeable clinicians are employing electroanalgesic treatment options for their patients with acute and/or chronic pain conditions.
Physicians are now finding that Electroanalgesa (EA) treatment is a valued option or adjunct to drug therapy, which alone can be ineffective, costly, addictive, and can cause undesired side effects such as gastro-intestinal irritation.
Looking forward, hundreds of medical researchers world- wide are currently investigating electroanalgesic medical treatment for the treatment of the pain associated with carpal tunnel syndrome, pain associated with fibromyalgia, pain associated with sciatica, and many other acute and/or chronic disorders.
Specific medical research organizations, universities, medical schools, and medical journals are documenting hopeful electroanalgesic medicine advances.
We have come a long way since Socrates’ colleagues placed electric eels in foot baths to ease pain. We have advanced well beyond T.E.N.S. Clinical electroanalgesic medicine is now a well documented path where clinicians break the limitations of drug therapy and surgery to find comfort for their patients.
More than 40 million people in the United States are affected with musculoskeletal pain, resulting in more than 300 million physician visits and costing hundreds of millions of dollars each year. Overall, approximately 50% to 60% of the US population is either partially, totally, temporarily or permanently disabled. Over 400 million workdays are lost each year due to some kind of pain.
The expected outcome of this targeted electroanalgesic procedure is the reduction in the ability of the affected nerves to transmit pain signals and, at the same time, promote healing by means of the depolarization effects on the nerve cells. The depolarization effect is accomplished by an advanced computer assisted High Definition frequency generator (HDfg) to reduce the hyper-irritated state of the nerves (8,300-10,000 pps).
Depending upon the individual patient and their medical condition, a diagnosis is made by the physician and a treatment plan is prescribed. The physician will then select the proper treatment parameters and the proper dosage level.
Initially, patients may experience some nervousness about electroanalgesic treatment. This is due to their assumptions of what electricity probably “feels like” and their overall fear associated with any medical procedure. However, once patients have experienced this advanced electroanalgesic treatment, their initial fears usually disappear and their comments about what electroanalgesic “feels like” refer to a “mild vibration sensation.” With proper dosage, patients report an enjoyable and pleasurable experience.
Q Are there any side effects?
A There are minimal side effects associated with electroanalgesic treatment. Depending upon the individual and their medical condition, possible side effects may be; relaxed or fatigued sensation, mild headache, increased bowel activity, increase in sexual arousal, original pain seems to move to new location, and muscle soreness. High electrical current dosages may cause a topical burn. Discuss this situation with your physician immediately.
Q How many treatments are necessary?
A Some pain management treatment regimens are similar to drug treatment regimens. It normally takes about 5-15 treatments, depending on the individual medical condition. Typically, the clinician will ask you to receive pain management treatments daily for the first 3-5 treatments, then 3 times per week for the next 2-3 weeks. Normal treatment time varies between 15-25 minutes. It is extremely important to complete the regimen prescribed by your physician. Patient compliance affects treatment outcome. Your concern should be discussed with your doctor, but it is recommended that you follow the complete regimen for optimum results.
Q I have had 3 treatments and still I have pain. Should I continue the treatments?
A Discuss this with your physician. Your physician may want to changethe treatment protocol indicated. In many pain syndromes, electroanalgesic treatments are very successful, however, there is no guarantee of success. Results have shown that 20-25% of patients will claim they received little or no long-term pain relief. For this reason, other treatment options should be added or considered. Sometimes the treatment success can be more subtle than other therapeutic methods. You should discuss your options with your physician should you elect not to complete the prescribed treatment regimen.
In no case, and at no time, should the patient ever experience a burning or stinging sensation from the treatment under the electrodes. If a burning or stinging sensation is felt notify the clinician immediately!
Q Are these treatments invasive?
A No, they are not invasive. The treatments are performed by placing the surface electrodes over specific areas of the body.
Q My treatment was combined with a device, or suction cups. I enjoyed the massage, but it left some red rings on the skin under the suction cups. Was I burned, and is this harmful?
A No. With some skin types, especially a fair complexion, a suction-induced redness might be produced, but this is temporary and will disappear shortly. The redness indicates an increase of blood flow to the area. Not only does the vacuum feel good, it produces a rapid increase of blood circulation under the electrodes and helps the electrical current enter the body.
Q This has really helped me. How can I get additional information for my family?
A Pain management medical Devices are sold to physicians only. Ask your physician for additional information or visit our web-site: www.NeuroMedinc.com for more information on this advance treatment.
Contraindications: Thrombophlebitis, manifest thrombosis, cardiac demand pacemaker, acute danger of hemorrhage, disturbances In cardiac rhythm, in cases of tentany-exercise caution in dosing, acute local inflammatory processes caused by bacterial or viral Infections. Do not stimulate over carotid sinus. Use adequate precautions in persons with suspected heart problems. epilepsy. or in higher-intensity transthoracic applications. Use precaution following recent surgical procedures when muscle contractions may disrupt the healing process and/or over the menstruating uterus.
Caution: Federal law restricts this device to sale by or on the order of a licensed physician or other practitioner licensed by law. See instruction manual for full warnings, precautions, and contraindications. High dosage may cause dermal burns. Effectiveness is highly dependent upon patient selection by a person qualified in the management of pain patients. Please review the Instruction manual carefully prior to use.
